
Mille Lacs Health System in Onamia (shown above) has seen an increase in heroin use, OD deaths and opioid addiction rates. This fall, two St. Kate's MPAS students will participate in a class that partners with the hospital to research alternative pain management treatments. Photo by Mary Rain.
The problem of opioid abuse
With an estimated 72,000 Americans who died from drug overdoses in 2017, according to the Center for Disease Control, opioid abuse continues to be a deadly drug epidemic.
What are opioids and why are they dangerous?
Opioids are a type of synthetic pain-relieving drugs, typically prescribed by a physician. Though opioid medications manage pain by inducing feelings of pleasure, the desire to continue experiencing those feelings can lead to addiction. Made illegally, synthetic opioids such as heroin and fentanyl are cut with other drugs and unknown properties, making illegal opioids cheaper, stronger, and more dangerous.
“Many patients are dependent, if not addicted, to these medications just due to the length of time that they have been taking them,” Mary Rains reported in the Mille Lacs Messenger. “Current research shows both the highly addictive nature of opioids, as well as the potential for increased pain, negative side effects and death.” Unfortunately, this information was not well understood by providers just a few years ago.
“The paradigm has shifted in thinking that we, as medical providers, had a responsibility to eliminate patients’ pain, to now understanding that the opioid medications that were once thought to be safe, are hurting our patient population through dependence and addiction; ironically, without improving chronic pain,” said Beth Twite ‘07, PA-C, MPAS'15.
Twite is 2015 graduate of St. Kate’s master of physician assistant studies (MPAS) program and joined Mille Lacs Health System (MLHS) as a physician assistant in 2016. She explained that a rural health system like MLHS in Onamia, Minnesota has limited resources to help patients struggling with chronic pain.
Students addressing the opioid epidemic
This fall, St. Kate’s MPAS students will participate in a required class titled, “Community and Clinical Quality Improvement.” The goal of the course is to develop skills “that can lead to improved patient care, increased efficiencies in organizational systems, reduced costs for patients and providers, and contribute to reductions in health care disparities,” shared Kari Hartwig, DrPH, the assistant professor leading this community-centered course.
Partnering with a clinic or community organization, students will provide assistance in a project where they can develop systems or improve efficiencies. MPAS students Travis Green and Bess Kuzma will be working under the direction of Twite and the pain committee within MLHS.
Twite’s relationship with St. Kate’s MPAS program has opened the door for St. Kate’s students as well as MLHS to benefit from high quality projects. “The [Community and Clinical Quality Improvement] projects are perfect for our location and really help students experience the different issues that rural patient populations face, while giving back to the community,” said Twite.
Green and Kuzma are in their third year in MPAS program and both completed their clinical rotations at MLHS. After being exposed to the especially large opioid problem in the area, Green emphasized just how close to home the overdose issue is.
MLHS has seen the number of patients in the ER for overdose almost triple from 25 patients in 2015 to 70 in 2017. While it’s clear that the method to treat chronic pain must change, decreasing opioid usage in those who have already been prescribed large quantities of opioids is not a quick or easy solution.
Today’s research shows that long-term treatment with opioids can have a hypersensitive effect where pain is felt more intensely than it would have been in the first place, making opioid treatment less effective overall. “Couple this realization with the fact that opioids are highly addictive and can often lead to abuse,” observed Green. “You now have this large push to decrease opioid usage nationally and are left with the puzzle of how to decrease usage in people who are already being prescribed large quantities of opioids.”
Green also explained that many patients are wary of decreasing their opioid usage because, biochemically, it can take months for a patient to be able to tolerate a decrease in dose. “The purpose of our research is to gauge the patients’ interest in alternative pain management therapies that may assist them in decreasing their opioid dose and allowing them non-pharmacologic methods of managing their pain,” explains Green. Examples of alternative services include acupuncture and massage.
Green and Kuzma will collect data for approximately two months, starting in September. They will present their findings to MLHS’s medical executives board and the pain committee members at the end of their study.
Students like Green and Kuzma aren’t just studying pressing issues like the opioid epidemic, they’re facing them head on and changing the future of treatment.
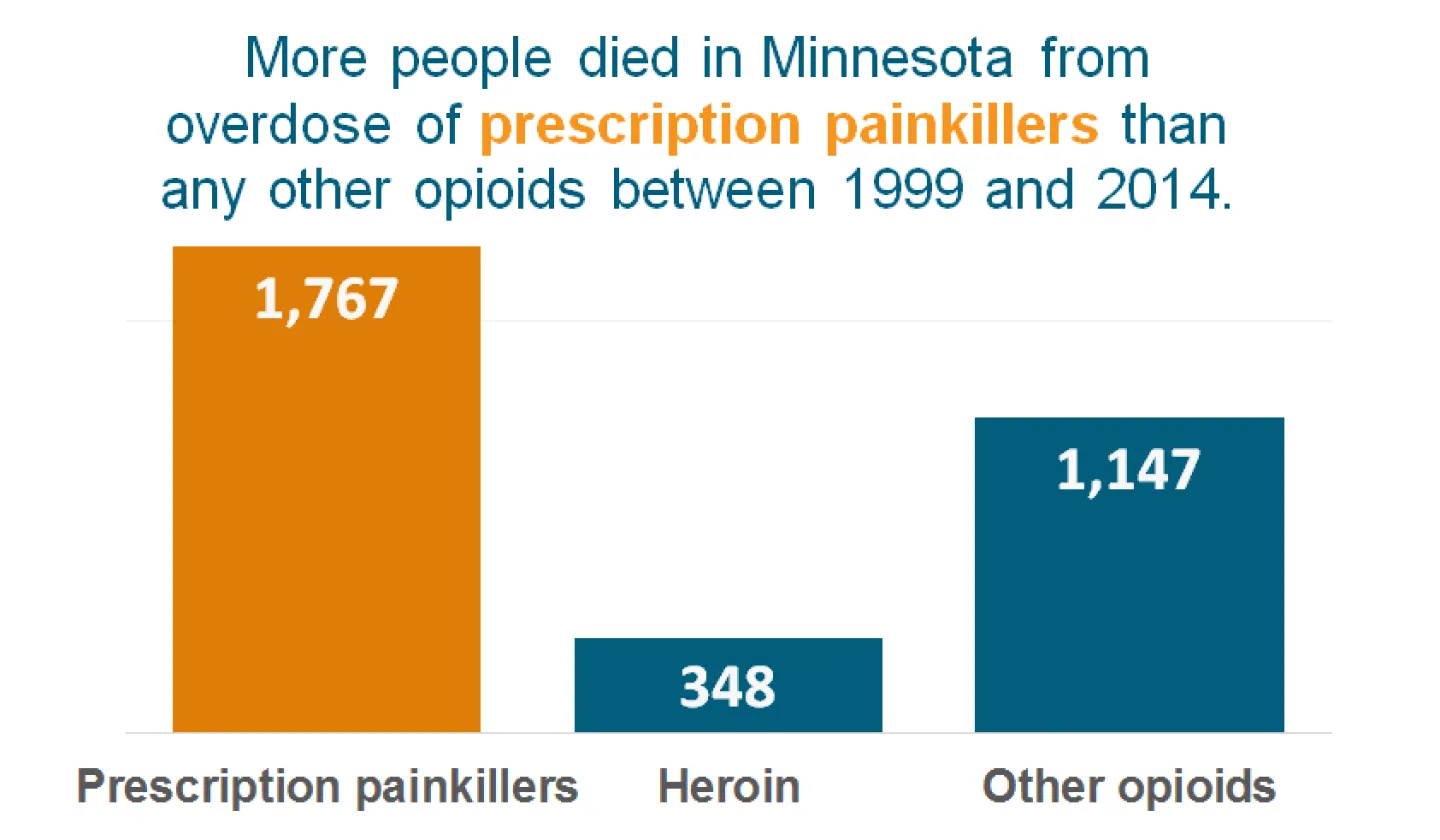
MPR News graphic. Source: Center for Disease and Control Prevention.
MLHS has seen the number of patients in the ER for overdose almost triple from 25 patients in 2015 to 70 in 2017. While it’s clear that the method to treat chronic pain must change, decreasing opioid usage in those who have already been prescribed large quantities of opioids is not a quick or easy solution.
Today’s research shows that long-term treatment with opioids can have a hypersensitive effect where pain is felt more intensely than it would have been in the first place, making opioid treatment less effective overall. “Couple this realization with the fact that opioids are highly addictive and can often lead to abuse,” observed Green. “You now have this large push to decrease opioid usage nationally and are left with the puzzle of how to decrease usage in people who are already being prescribed large quantities of opioids.”
Green also explained that many patients are wary of decreasing their opioid usage because, biochemically, it can take months for a patient to be able to tolerate a decrease in dose. “The purpose of our research is to gauge the patients’ interest in alternative pain management therapies that may assist them in decreasing their opioid dose and allowing them non-pharmacologic methods of managing their pain,” explains Green. Examples of alternative services include acupuncture and massage.
Green and Kuzma will collect data for approximately two months, starting in September. They will present their findings to MLHS’s medical executives board and the pain committee members at the end of their study.
Students like Green and Kuzma aren’t just studying pressing issues like the opioid epidemic, they’re facing them head on and changing the future of treatment.
By Amy Mullowney '19